Berdazimer
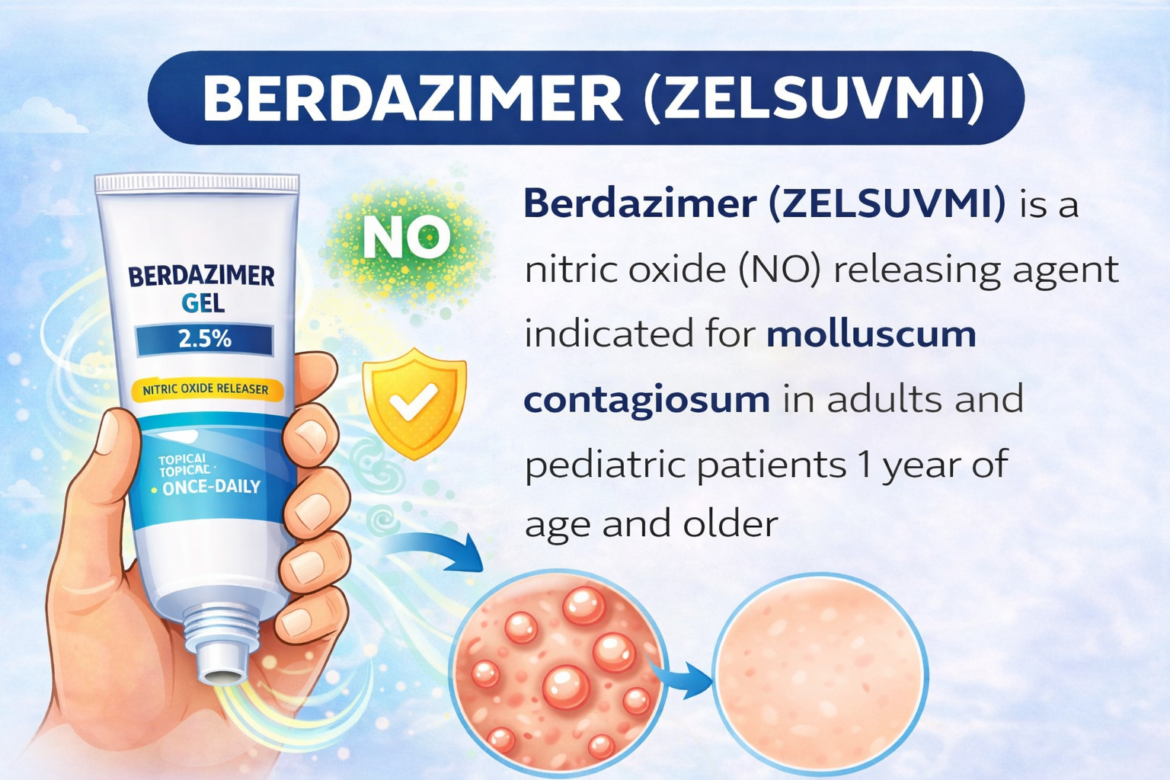
A first-in-class topical nitric oxide (NO) releasing agent consisting of berdazimer sodium gel (Tube A) mixed with a proton-donating hydrogel (Tube B) immediately before application. The first and only FDA-approved prescription topical treatment specifically indicated for molluscum contagiosum (MC) — a highly transmissible poxvirus infection predominantly affecting children — with established efficacy and a favorable systemic safety profile based on subnanomolar systemic exposure under maximal use conditions.
Drug Overview
NDA 217424Mechanism of Action
Section 12.1ZELSUVMI is a nitric oxide (NO) releasing agent. Berdazimer sodium (NVN1000) is a macromolecular silica-based polymer backbone with covalently bound diazeniumdiolate moieties that release nitric oxide upon protonation. When the berdazimer gel (Tube A) is mixed with the proton-donating hydrogel (Tube B), NO is released locally at the site of MC lesions. Nitric oxide is a highly reactive signaling molecule with antimicrobial, antiviral, and immunomodulatory properties across a broad concentration spectrum. The precise mechanism by which NO exerts its effect on the molluscum contagiosum virus (MCV) is unknown per the prescribing information.
Therapeutic Landscape — Topical Therapies for Molluscum Contagiosum
| Agent | Class / MOA | Route | Status (US) | Notes |
|---|---|---|---|---|
| Berdazimer (ZELSUVMI) | NO releasing agent (topical) | Topical QD ×12 wk | FDA Jan 5, 2024 (NDA 217424) | First FDA-approved Rx topical for MC; ≥1 year |
| Cantharidin (Ycanth) | Mitotic inhibitor (vesicant) | Topical in-office | FDA Jul 26, 2023 (NDA 212905) | HCP-administered; ≥2 years; blistering mechanism |
| Imiquimod 5% (Zyclara/generic) | TLR7/8 agonist (immune modulator) | Topical 3×/wk | Off-label (FDA approved for genital warts/AK) | No FDA indication for MC; used off-label |
| Podophyllotoxin (generic) | Antimitotic (off-label) | Topical | Off-label | Not evaluated in randomized MC trials |
| Curettage / Cryotherapy | Procedural (destructive) | In-office procedure | Standard of care (no FDA approval required) | Painful in children; risk of scarring; no controlled trials |
Source: FDA Prescribing Information NDA 217424, Ref ID 5304861. FDA Multi-disciplinary Review NDA 217424, Ref ID 5304936. Competitive landscape based on FDA approval records. Berdazimer was developed under IND 137015. Prior to ZELSUVMI approval, no FDA-approved prescription topical therapy existed specifically for molluscum contagiosum.
Baseline & Trial Characteristics
Table 20–22, NDA 217424 Medical ReviewTrial Design Summary
Section 8.1.1| Parameter | NI-MC301 | NI-MC302 | NI-MC304 (Pivotal) |
|---|---|---|---|
| NCT Number | NCT03927716 | NCT03927703 | NCT04535531 |
| Randomization | 2:1 (SB206:vehicle) | 2:1 (SB206:vehicle) | 1:1 (SB206:vehicle) |
| Sample Size | N=352 (236 / 116) | N=355 (237 / 118) | N=891 (444 / 447) |
| No. of Centers | 33 (all US) | 33 (all US) | 55 (all US) |
| Primary Endpoint | Complete clearance Wk 12 | Complete clearance Wk 12 | Complete clearance Wk 12 |
| Key Secondary Endpoint | Complete clearance Wk 8 | Complete clearance Wk 8 | Complete clearance Wk 8 |
| Stratification | Investigator type; household | Investigator type; household | + Baseline BOTE score added |
| Missing Data Method | NRI (conservative) | NRI (conservative) | NRI (balanced dropout) |
| Conduct Period | 2019–2020 | 2019–2020 | 2020–2022 (COVID era) |
| Remote Visits | No | No | Week 4 allowed remotely |
| Efficacy Conclusion | Not significant (p=0.3637) | Marginal (p=0.0510) | Significant (p<0.0001) ✓ |
Demographic Characteristics (NI-MC304 ITT, N=891)
Table 20| Characteristic | Berdazimer (N=444) | Vehicle (N=447) |
|---|---|---|
| Mean age (SD), years | 6.6 (4.50) | 6.5 (4.34) |
| Median age (range) | 5.6 (0.9–47.5) | 6.0 (1.3–49.0) |
| Age <2 years, n (%) | 16 (3.6%) | 12 (2.7%) |
| Age 2–<6 years, n (%) | 220 (49.5%) | 213 (47.7%) |
| Age 6–<12 years, n (%) | 178 (40.1%) | 201 (45.0%) |
| Age 12–<18 years, n (%) | 24 (5.4%) | 15 (3.4%) |
| Age ≥18 years, n (%) | 6 (1.4%) | 6 (1.3%) |
| Female, n (%) | 216 (48.6%) | 234 (52.3%) |
| White, n (%) | 387 (87.2%) | 382 (85.5%) |
| Black or African American, n (%) | 21 (4.7%) | 28 (6.3%) |
| Hispanic or Latino, n (%) | 94 (21.2%) | 87 (19.5%) |
Baseline Disease Characteristics (NI-MC304 ITT)
Table 21| Characteristic | Berdazimer (N=444) | Vehicle (N=447) |
|---|---|---|
| Mean baseline lesion count (SD) | 23.1 (17.60) | 20.5 (16.18) |
| Median lesion count (range) | 18.5 (3–70) | 15.0 (3–69) |
| <20 lesions, n (%) | 229 (51.6%) | 267 (59.7%) |
| ≥20 lesions, n (%) | 215 (48.4%) | 180 (40.3%) |
| Mean time since onset (months) | 12.0 | 13.1 |
| Baseline BOTE score = 0 (no inflammation), n (%) | 225 (50.7%) | 222 (49.7%) |
| Baseline BOTE ≥1 (mild–very severe), n (%) | 219 (49.3%) | 225 (50.3%) |
| AD/eczema history, n (%) | 67 (15.1%) | 56 (12.5%) |
| Dermatologist investigator, n (%) | 260 (58.6%) | 265 (59.3%) |
| Mean treatment compliance (%) | 91.4% | 94.8% |
Source: NDA 217424 Multi-disciplinary Review, Ref ID 5304936. BOTE = Beginning-of-the-End (clinical sign of impending spontaneous resolution). NI-MC304 had higher baseline lesion counts in the berdazimer arm vs vehicle (23.1 vs 20.5) due to randomization imbalance. Compliance lower in active arm, consistent with application site reaction–driven interruptions. All three trials conducted at US centers only.
Clinical Efficacy
Section 14 / Table 2 (Label); Table 25 (Medical Review)Complete Clearance Rates — All Three Trials
ITT Population, GEE Logistic Regression55 US centers; stratified by investigator type, household size, and BOTE score. Primary endpoint met with high statistical significance.
Week 12 — Complete Clearance Rate (Primary)
Week 8 — Complete Clearance Rate (Key Secondary)
Marginally missed primary endpoint significance threshold; conservative NRI with higher missing data in active arm (16% vs 12.7%). Multiple sensitivity analyses and Week 8 secondary were supportive. FDA concluded efficacy demonstrated.
Week 12 — Complete Clearance Rate (Primary)
Week 8 — Complete Clearance Rate (Key Secondary)
Failed to demonstrate efficacy on primary endpoint. Highly imbalanced missing data (16.1% berdazimer vs 3.4% vehicle) with conservative NRI likely attenuated the treatment effect. Small trend favoring active treatment. Results do not detract from the overall efficacy evidence.
Week 12 — Complete Clearance Rate (Primary)
Efficacy Summary Table
Table 25, NDA 217424 Medical Review (Label Table 2)| Endpoint | NI-MC304 Berdazimer (N=444) | NI-MC304 Vehicle (N=447) | Treatment Difference (95% CI) | NI-MC302 Berdazimer (N=237) | NI-MC302 Vehicle (N=118) | Treatment Difference (95% CI) |
|---|---|---|---|---|---|---|
| Complete Clearance Wk 12 (Primary) | 32.4% | 19.7% | +12.8% (7.1%, 18.6%) p<0.0001 | 30.0% | 20.3% | +9.2% (−0.04%, 18.4%) p=0.0510 |
| Complete Clearance Wk 8 (Key Secondary) | 19.6% | 11.6% | +7.5% (3.0%, 12.0%) p=0.0012 | 13.9% | 5.9% | +7.8% (1.8%, 13.8%) |
| Complete Clearance Wk 12 (NI-MC301) | 25.8% (N=236) | 21.6% (N=116) | +4.3% (−5.0%, 13.6%) p=0.3637 — Not significant | |||
Source: FDA Prescribing Information NDA 217424 (label Table 2) and NDA 217424 Multi-disciplinary Review, Ref ID 5304936 (Table 25). Complete clearance defined as total MC lesion count = 0 at assessment. GEE = generalized estimating equation; NRI = non-responder imputation; ITT = intent-to-treat. Note: “complete clearance” is a stringent endpoint — partial clearance data (≥90% reduction, change in lesion count) consistently favored active treatment across all three trials.
Safety Profile
Section 6.1 (Label); Integrated Summary of Safety (ISS)Adverse Reactions ≥1% (Pooled Trials 1, 2, 3 — Label Table 1)
Day 1 through Week 12; Treatment Emergent Adverse Events| Adverse Reaction | ZELSUVMI N=916 | Vehicle N=680 | Total Berdazimer (%) | ||||
|---|---|---|---|---|---|---|---|
| Mild | Moderate | Severe | Mild | Moderate | Severe | ||
| Any TEAE | 220 (24.0%) | 192 (21.0%) | 16 (1.7%) | 118 (17.4%) | 47 (6.9%) | 4 (0.6%) | 46.7% |
| Application Site Pain† (burning/stinging) | 113 (12.3%) | 56 (6.1%) | 2 (0.2%) | 30 (4.4%) | 3 (0.4%) | 0 | 18.7% |
| Application Site Erythema | 48 (5.2%) | 55 (6.0%) | 4 (0.4%) | 7 (1.0%) | 2 (0.3%) | 0 | 11.7% |
| Application Site Pruritus | 36 (3.9%) | 15 (1.6%) | 1 (0.1%) | 5 (0.7%) | 2 (0.3%) | 0 | 5.7% |
| Application Site Exfoliation | 18 (2.0%) | 26 (2.8%) | 2 (0.2%) | 0 | 0 | 0 | 5.0% |
| Application Site Dermatitis | 16 (1.7%) | 26 (2.8%) | 3 (0.3%) | 3 (0.4%) | 2 (0.3%) | 0 | 4.9% |
| Application Site Swelling | 17 (1.9%) | 14 (1.5%) | 1 (0.1%) | 3 (0.4%) | 1 (0.1%) | 0 | 3.5% |
| Pyrexia | 14 (1.5%) | 6 (0.7%) | 0 | 6 (0.9%) | 1 (0.1%) | 0 | 2.3% |
| Application Site Erosion | 7 (0.8%) | 5 (0.5%) | 3 (0.3%) | 1 (0.1%) | 0 | 0 | 1.6% |
| Application Site Discoloration | 13 (1.4%) | 1 (0.1%) | 0 | 1 (0.1%) | 0 | 0 | 1.5% |
| Application Site Vesicles | 5 (0.5%) | 9 (1.0%) | 0 | 0 | 1 (0.1%) | 0 | 1.5% |
| Application Site Irritation | 7 (0.8%) | 4 (0.4%) | 0 | 0 | 0 | 0 | 1.2% |
| Application Site Infection | 4 (0.4%) | 4 (0.4%) | 2 (0.2%) | 2 (0.3%) | 1 (0.1%) | 0 | 1.1% |
† Application site pain includes burning and stinging sensations. Adverse reactions reported ≥1% of subjects and more frequently than vehicle. Source: FDA label NDA 217424 Table 1, Ref ID 5304861.
Warnings & Precautions
Section 5.1- Application Site Reactions incl. Allergic Contact Dermatitis (Section 5.1): Suspect allergic contact dermatitis if pain, pruritus, swelling, or erythema persists at the application site for >24 hours. Discontinue ZELSUVMI and initiate appropriate therapy if allergic contact dermatitis occurs.
Key Safety Considerations
Discontinuation Due to TEAEs
Higher dropout rates in the berdazimer arm across trials NI-MC301 and NI-MC302 were predominantly due to withdrawn consent/assent and lost to follow-up — not adverse events per se. Only 5 subjects (1.1%) in NI-MC304 discontinued due to adverse events vs. 3 (0.7%) in vehicle. Application site reactions were manageable and did not generate a systematic discontinuation signal.
Source: NDA 217424 label Table 1 (Ref ID 5304861) and NDA 217424 Medical Review (Ref ID 5304936). No contraindications identified. No drug-drug interaction studies conducted; not warranted given subnanomolar systemic exposure.
Pharmacology & Pharmacokinetics
Section 12 / Table 15 (NDA 217424 Medical Review)PK Summary Table (hMAP3 as Structural Marker)
Table 15 / Table 49, NDA 217424 Medical Review| PK Parameter | Details |
|---|---|
| Analyte | hMAP3 (hydrolyzed N-methylaminopropyl-trimethoxysilane) — specific structural marker for berdazimer sodium backbone. Also: plasma nitrate ion (NO metabolism), methemoglobin (systemic NO exposure biomarker) |
| Bioanalytical method | High-performance LC/MS/MS; LLOQ 5 ng/mL for hMAP3, 300 ng/mL for nitrate |
| Study population | NI-MC101: N=34 children aged 2–12 years with MC; maximal use field treatment (484 cm²) |
| hMAP3 Day 1 | 0/34 subjects had quantifiable concentrations (all <LLOQ of 5 ng/mL) |
| hMAP3 Day 15 | 2/34 subjects had quantifiable concentrations; Cmax: 5.12 and 33.9 ng/mL; Tmax ~2 h; AUC0–3 = 75.5 h·ng/mL (1 subject) |
| Accumulation | No accumulation detected (plasma hMAP3 exposure not appreciably accumulating after 5 daily topical administrations — confirmed in animal models) |
| Plasma nitrate | Levels remained stable at background/endogenous levels across Days 1 and 15; no treatment-related increase |
| Distribution | Not conducted; topical product applied directly to target site. Plasma protein binding in humans not determined. |
| Metabolism / Excretion | No formal studies conducted (not deemed necessary given negligible systemic exposure) |
| Drug-drug interactions | No DDI studies conducted; not warranted due to subnanomolar systemic exposure |
| QTc | No clinically relevant QTc prolongation observed in dedicated QT study (SB204 12% gel, ~33× expected MC treatment area) |
| Dose proportionality | Not assessed in clinical studies |
| Therapeutic individualization | Not applicable — topical product applied locally; low systemic exposure precludes PK-guided dosing |
Mechanism of Action & Pharmacology
Section 12.1 / Non-Clinical ReviewBerdazimer sodium (NVN1000) is a macromolecular silasesquioxane polymer with covalently bound diazeniumdiolate (NONOate) moieties that release nitric oxide upon contact with protons. In the two-tube system, when the berdazimer sodium gel (Tube A) is mixed with the proton-donating hydrogel (Tube B), protonation of the NONOate groups triggers NO release directly at the skin surface. NO is a highly reactive diatomic radical with established antimicrobial, antiviral, and immunostimulatory properties. At low/signaling concentrations, NO activates guanylate cyclase and modulates immune responses; at higher concentrations it exerts cytotoxic effects via reactive nitrogen species. The exact mechanism by which this NO release clears molluscum contagiosum virus (MCV, a poxvirus) lesions is not established.
Source: NDA 217424 Clinical Pharmacology Review (Section 6.2.2, Table 15), Non-Clinical Review (Section 5), and Label Section 12. Phase 1 maximal use PK study NI-MC101: open-label, N=34, ages 2–12 years. All US centers. OCP review completed by Division Director Suresh Doddapaneni (OCP). No outstanding Clinical Pharmacology issues precluded approval.
Dosing, Administration & Precautions
Section 2, 4, 5 / LabelPreparation & Administration Instructions
Section 2.1 / 2.2Preparation Steps
- Place Dosing Guide on a clean, flat surface.
- Remove cap from Tube A (blue label, berdazimer gel). Squeeze gel onto the blue lane of the Dosing Guide to cover the entire area. Replace cap on Tube A tightly.
- Remove cap from Tube B (yellow label, hydrogel). Squeeze gel onto the yellow lane of the Dosing Guide to cover the entire area. Replace cap on Tube B tightly.
- Using a fingertip, mix both gels in the center of the Dosing Guide with circular motion while counting to 20. Clumping during mixing is normal.
- Apply the mixed gel immediately to MC lesions. Do not store mixed gel.
Post-Application Instructions
- Apply an even, thin layer over each MC lesion including new lesions.
- Allow ZELSUVMI to dry for 10 minutes before dressing/clothing application to skin.
- Avoid swimming, bathing, or washing the treated areas for 1 hour after application.
- Wash hands after application (unless hands are being treated).
- Avoid application to uninvolved skin; avoid transfer to eyes.
- For topical use only. Not for ophthalmic, oral, or intravaginal use.
Storage Instructions
- Prior to dispensing: Refrigerate at 2°C–8°C (36°F–46°F) until dispensed.
- After dispensing: Store at room temperature 20°C–25°C (68°F–77°F) in a dry location.
- Discard 60 days after removal from refrigeration.
- Do not freeze. Keep away from open flame (product contains alcohol).
- Do not premix or store mixed ZELSUVMI.
How Supplied (Section 16)
- Carton NDC: 71403-103-31
- Tube A (14 g, blue label): Berdazimer sodium gel. NDC 71403-113-14. 240 mg berdazimer sodium/g gel.
- Tube B (17 g, yellow label): Hydrogel (translucent to opaque white). UPC 71403-0000-17.
- Dosing Guide: Included in carton; reusable — do not discard.
Warnings & Precautions
Section 5- Application Site Reactions including Allergic Contact Dermatitis (5.1): Application site reactions have occurred in ZELSUVMI-treated patients. Suspect allergic contact dermatitis if pain, pruritus, swelling, or erythema at the application site persists for longer than 24 hours. If allergic contact dermatitis occurs: discontinue ZELSUVMI and initiate appropriate therapy. Application site reactions were the most common reason for clinician review of treatment.
Special Populations
Section 8| Population | Guidance |
|---|---|
| Pregnancy (8.1) | No human pregnancy data. Animal oral studies showed fetal malformations only at doses causing severe maternal toxicity (rats: 189 mg/kg/day; rabbits: 284 mg/kg/day). Clinical relevance unknown given subnanomolar topical systemic exposure vs. oral bioavailability. |
| Lactation (8.2) | No data on presence of berdazimer or metabolites in human or animal milk. Consider developmental benefits of breastfeeding alongside maternal need for treatment. |
| Pediatric Use (8.4) | Safety and efficacy established for patients ≥1 year. 1,575 pediatric subjects in trials (904 berdazimer); includes 29 subjects <2 years (1 subject <1 year). Not established in infants <1 year. |
| Geriatric Use (8.5) | Of ZELSUVMI-treated subjects in clinical trials, none were 65–74 years of age; 1 was ≥75 years. Insufficient data to determine whether elderly respond differently from younger adults. |
| Renal/Hepatic Impairment | Not studied. Given negligible systemic exposure, dose adjustment not expected to be required. |
Source: FDA Prescribing Information NDA 217424, Ref ID 5304861, Revised 01/2024. Manufactured for EPIH SPV, LLC, Wilmington, Delaware 19801. U.S. Patents: www.novan.com/patents. Patient information line: 1-855-330-7546. For SUSPECTED ADVERSE REACTIONS contact LNHC, Inc. at 1-800-499-4468 or FDA MedWatch at 1-800-FDA-1088.
Regulatory History
NDA 217424 — 505(b)(1) Standard ReviewRegulatory Timeline
Regulatory Considerations & Supporting Evidence
| Aspect | Detail |
|---|---|
| Application number | NDA 217424 (Orig1s000) |
| IND number | IND 137015 (shared with SB204 acne program) |
| Applicant | EPIH SPV, LLC, Wilmington, Delaware 19801 (originally developed by Novan, Inc. — code name NVN1000 / SB206) |
| Pivotal trial(s) | NI-MC304 (NCT04535531) — primary adequate and well-controlled trial; NI-MC302 (NCT03927703) — supportive adequate and well-controlled trial |
| Failed trial | NI-MC301 (NCT03927716) — did not demonstrate efficacy; conservative NRI with imbalanced dropout; does not detract from overall evidence |
| Statistical standard | Two adequate and well-controlled trials (21 CFR 314.126(a)(b)); FDA concluded substantial evidence of effectiveness was demonstrated by NI-MC304 and NI-MC302 |
| Primary endpoint accepted | Complete clearance (lesion count = 0) at Week 12 — FDA-endorsed dichotomous endpoint for MC; partial clearance endpoints not accepted for labeling |
| Systemic tox waiver | 6-month systemic rodent repeat-dose toxicology study waived; 1-year chronic systemic rodent toxicology and pre/post-natal development study waived — based on subnanomolar systemic exposure at maximal clinical use |
| Nonclinical toxicology status | 2-year mouse dermal carcinogenicity study (up to 4% berdazimer): no drug-related tumor findings. Ames assay positive (mutagenic) but in vitro and in vivo clastogenicity assays negative. |
| Reference ID (label / review) | 5304861 (prescribing information) / 5304936 (multi-disciplinary review) |
| U.S. Patents | www.novan.com/patents |
Source: NDA 217424 Multi-disciplinary Review, Ref ID 5304936 (completed Jan 4, 2024). Label NDA 217424, Ref ID 5304861, Revised 01/2024. Section 505(b)(1) of the Federal Food, Drug and Cosmetic Act. All clinical trials conducted in the United States. Review conducted by Division of Dermatology and Dentistry (DDD), Office of Immunology and Inflammation (OII), CDER, FDA.