Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124

Clarity in Trials, Confidence in Decisions

Clarity in Trials, Confidence in Decisions
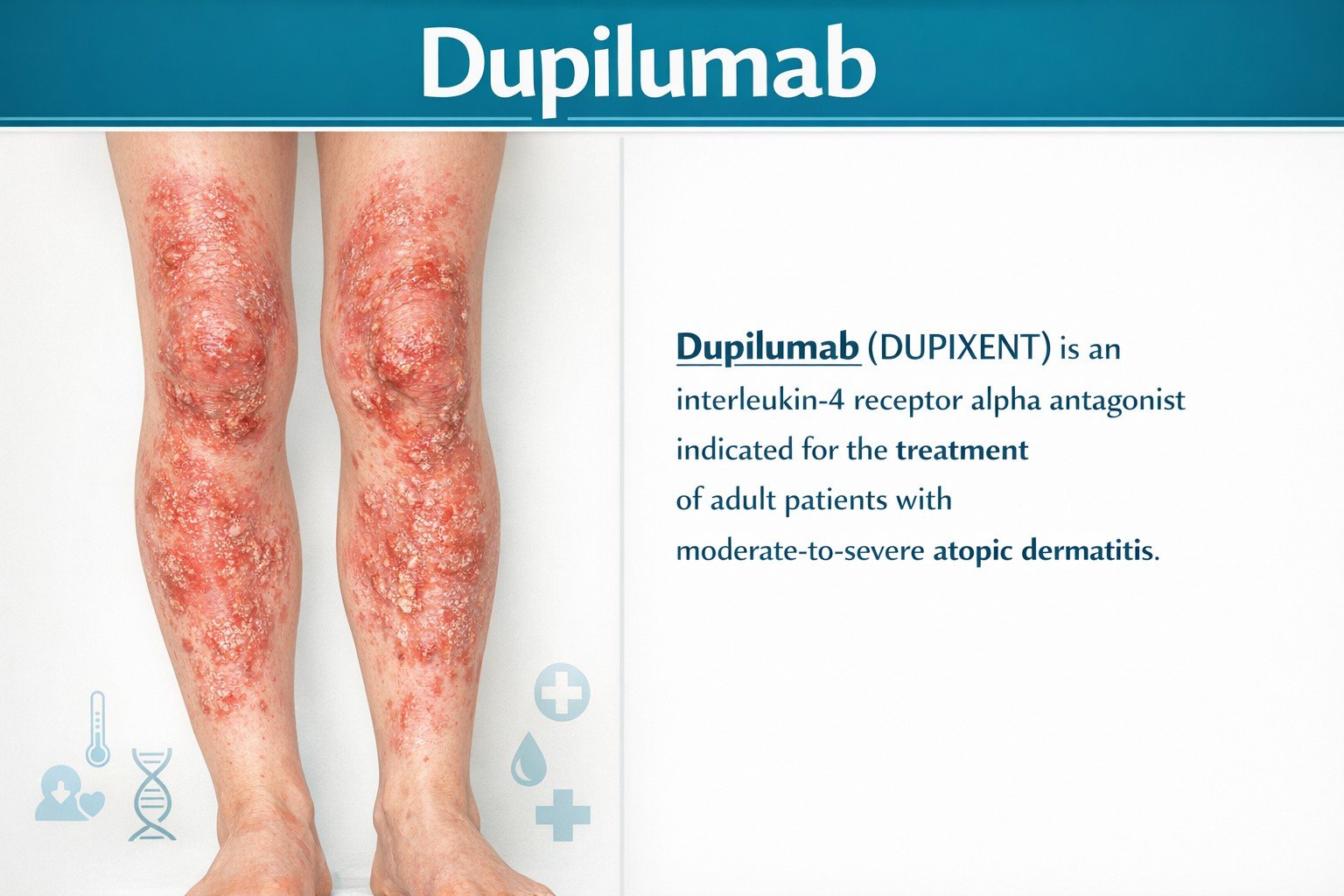
Treatment of adult patients with moderate-to-severe atopic dermatitis whose disease is not adequately controlled with topical prescription therapies or when those therapies are not advisable. May be used with or without topical corticosteroids.
| Study | Design | N | Duration | Key Intervention |
|---|---|---|---|---|
| SOLO 1 (1334) | R, DB, PC, MC | 671 | 16 weeks | Dupilumab 300 mg Q2W vs Placebo — monotherapy |
| SOLO 2 (1416) | R, DB, PC, MC | 708 | 16 weeks | Dupilumab 300 mg Q2W vs Placebo — monotherapy |
| CHRONOS (1224) | R, DB, PC, MC | 740 | 52 weeks | Dupilumab 300 mg Q2W + TCS vs Placebo + TCS |
R=randomized; DB=double-blind; PC=placebo-controlled; MC=multicenter; TCS=topical corticosteroids. All studies enrolled adults (≥18 years) with IGA ≥3, EASI ≥16, and BSA ≥10%. Source: BLA 761055, Clinical Review, Brenda Carr MD.
Atopic dermatitis affects approximately 3% of adults globally, with 10–30% of childhood-onset cases persisting into adulthood. The AD population is characterised by heightened Th2 immune polarisation with elevated IL-4, IL-13, IgE, and peripheral eosinophilia. At the time of dupilumab’s approval, the only FDA-approved systemic option was systemic corticosteroids, which are generally not recommended for long-term use. Dupilumab was the first targeted biologic approved for AD, and its approval represented a paradigm shift enabling cytokine-directed therapy in this indication.
The Phase 3 development program enrolled 2,119 subjects across the three pivotal trials. The primary endpoint — IGA 0/1 with ≥2-point improvement at Week 16 — was met with high statistical significance (p<0.0001) in all three trials. Dupilumab also substantially reduced pruritus (≥4-point NRS improvement) and EASI scores, and the safety profile was favourable, with conjunctivitis being the most notable drug-related adverse event signal.
| Characteristic | Dupilumab 300 mg Q2W | Placebo |
|---|---|---|
| Randomized (FAS) | 224 | 224 |
| Mean Age (yr) | 39.8 ± 14.7 | 39.5 ± 13.9 |
| Male | 130 (58%) | 118 (53%) |
| White / Asian / Black | 69% / 24% / 5% | 65% / 25% / 7% |
| IGA Moderate (3) / Severe (4) | 52% / 48% | 50% / 50% |
| Mean EASI score | 33.0 ± 13.6 | 34.5 ± 14.5 |
| Mean BSA involved (%) | 54.7 ± 23.2 | 57.5 ± 23.4 |
| Weekly Average Peak Pruritus NRS | 7.2 ± 1.9 | 7.4 ± 1.8 |
| Baseline NRS ≥4 | 213 (95%) | 212 (95%) |
| Characteristic | Dupilumab 300 mg Q2W | Placebo |
|---|---|---|
| Randomized (FAS) | 233 | 236 |
| Mean Age (yr) | 36.9 ± 14.0 | 37.4 ± 14.1 |
| Male | 137 (59%) | 132 (56%) |
| White / Asian / Black | 71% / 19% / 6% | 66% / 21% / 9% |
| IGA Moderate (3) / Severe (4) | 51% / 49% | 51% / 49% |
| Mean EASI score | 31.8 ± 13.1 | 33.6 ± 14.3 |
| Mean BSA involved (%) | 52.7 ± 21.2 | 54.3 ± 23.1 |
| Weekly Average Peak Pruritus NRS | 7.6 ± 1.6 | 7.5 ± 1.9 |
| Baseline NRS ≥4 | 225 (97%) | 221 (94%) |
| Characteristic | Dupilumab 300 mg Q2W + TCS | Placebo + TCS |
|---|---|---|
| Randomized (FAS) | 106 | 315 |
| Mean Age (yr) | 39.6 ± 14.0 | 36.6 ± 13.0 |
| Male | 62 (59%) | 193 (61%) |
| White / Asian / Black | 70% / 27% / 2% | 66% / 26% / 6% |
| IGA Moderate (3) / Severe (4) | 50% / 50% | 53% / 47% |
| Mean EASI score | 33.6 ± 13.3 | 32.6 ± 12.9 |
| Mean BSA involved (%) | 59.5 ± 20.8 | 56.9 ± 21.7 |
| Weekly Average Peak Pruritus NRS | 7.4 ± 1.7 | 7.3 ± 1.8 |
| Baseline NRS ≥4 | 102 (96%) | 299 (95%) |
Source: BLA 761055 Clinical Review, Tables 9, 10, 22, 23, 38, 39. Demographic and baseline disease characteristics were well-balanced across treatment arms in all three trials. The AD diagnosis required ≥3 years of chronic disease and was made using AAD Consensus Criteria (Eichenfield 2014).
| Response Pattern | Dupilumab Q2W + TCS (n=89) | Placebo + TCS (n=264) |
|---|---|---|
| Responder at Week 16 and Week 52 | 22% | 7% |
| Responder Week 16, Non-responder Week 52 | 20% | 7% |
| Non-responder Week 16, Responder Week 52 | 13% | 6% |
| Non-responder at both Week 16 and 52 | 44% | 80% |
| Overall Responder Rate at Week 52 | 36% | 13% |
Source: BLA 761055 Clinical Review (Brenda Carr, MD) and FDA-approved prescribing information. All percentages are FAS (all randomized). Subjects receiving rescue treatment or with missing data considered non-responders. CMH test stratified by baseline IGA severity and geographic region.
| Adverse Reaction | Dupi Mono Q2W N=529 | Placebo Mono N=517 | Dupi+TCS Q2W N=110 | Placebo+TCS N=315 |
|---|---|---|---|---|
| Injection site reactions | 10% | 5% | 10% | 6% |
| Conjunctivitis (cluster)† | 10% | 2% | 9% | 5% |
| Oral herpes | 4% | 2% | 3% | 2% |
| Other herpes simplex virus‡ | 2% | 1% | 1% | <1% |
| Eye pruritus | 1% | <1% | 2% | 1% |
| Blepharitis | <1% | <1% | 5% | 1% |
| Keratitis (cluster)§ | <1% | 0% | 4% | 0% |
| Dry eye | <1% | 0% | 2% | <1% |
† Conjunctivitis cluster includes allergic, bacterial, viral, giant papillary conjunctivitis, eye irritation, and eye inflammation.
‡ Herpes simplex cluster excludes eczema herpeticum.
§ Keratitis cluster includes keratitis, ulcerative, allergic, atopic keratoconjunctivitis, and ophthalmic herpes simplex.
Monotherapy data pooled from Trials 1334, 1416 (AD-1021). Source: FDA-approved prescribing information, March 2017.
| Parameter | 16-Week Monotherapy | 52-Week + TCS |
|---|---|---|
| Anti-drug antibody (ADA) development | ~7% (dupilumab) | ~7% (dupilumab+TCS) |
| Neutralizing ADA | ~30% of ADA+ ≈ 2% overall | ~14% of ADA+ ≈ 1% overall |
| Persistent antibody response | Not characterized | ~2% (≥2 consecutive positive samples) |
| Clinical impact | ADA associated with lower serum dupilumab concentrations; some high-titer ADA+ subjects had no detectable drug | Same pattern |
| Placebo ADA | ~2% | ~8% (placebo+TCS) |
Source: BLA 761055, FDA-approved prescribing information March 2017, Clinical Review Brenda Carr MD.
Dupilumab is a fully human IgG4 monoclonal antibody that specifically binds the IL-4Rα subunit. The IL-4Rα chain is shared between two distinct receptor complexes: the Type I receptor (IL-4Rα + γc, expressed on T cells, mast cells, basophils) which is the primary signalling complex for IL-4, and the Type II receptor (IL-4Rα + IL-13Rα1, expressed on non-haematopoietic cells including keratinocytes and fibroblasts) which mediates both IL-4 and IL-13 signalling. By blocking IL-4Rα with a single agent, dupilumab prevents both pathways simultaneously.
| Parameter | Details |
|---|---|
| Absorption | Slow subcutaneous absorption; Tmax ~1 week after single 600 mg load |
| Distribution | Low volume of distribution (~4.8 L); minimal tissue penetration as expected for large IgG molecule |
| Metabolism | Not formally characterized. Expected to undergo catabolism to small peptides and amino acids via standard IgG catabolic pathways |
| Elimination | Nonlinear (target-mediated drug disposition, TMDD). Exposure increases >dose-proportionally: 30-fold AUC increase for 8-fold dose increase (75→600 mg) |
| Dose linearity | Non-linear TMDD. At higher doses/steady-state, target saturation predominates and PK approaches linearity |
| Body weight effect | Higher body weight → lower trough concentrations. No dose adjustment required based on available data |
| Geriatric (≥65 yr) | Steady-state trough 69.4±31.4 µg/mL (Q2W). No dose adjustment required |
| Renal/Hepatic impairment | No formal studies conducted |
| Drug interaction studies | Not conducted with DUPIXENT |
Receptor blockade with dupilumab leads to predictable pharmacodynamic changes: serum IL-4 and IL-13 levels increase following treatment (consistent with ligand accumulation), while markers of type 2 inflammation — including TARC/CCL17, total IgE, and peripheral eosinophil count — decrease over the treatment period. In monotherapy trials, a transient initial rise in eosinophil counts was observed (not seen in TCS combination trial), with levels returning to near-baseline by Week 16.
| Property | Value |
|---|---|
| Class | Recombinant human IgG4 monoclonal antibody |
| Molecular target | IL-4Rα (interleukin-4 receptor alpha subunit) |
| Molecular weight | ~147 kDa |
| Production | Chinese Hamster Ovary (CHO) cell suspension culture, recombinant DNA technology |
| Formulation | Sterile, preservative-free, clear to slightly opalescent, colorless to pale yellow solution |
| Excipients | L-arginine hydrochloride (10.5 mg), L-histidine (6.2 mg), polysorbate 80 (4 mg), sodium acetate (2 mg), sucrose (100 mg), water for injection; pH 5.9 |
| Presentation | 300 mg/2 mL single-dose pre-filled syringe (with or without needle shield); 2.25 mL siliconized Type-1 clear glass; non-latex needle cap |
Source: BLA 761055 prescribing information Section 12, Clinical Pharmacology. No formal drug interaction studies have been conducted. CYP450 monitoring warranted for narrow-TI substrates.
| Form | Strength | NDC |
|---|---|---|
| Single-dose pre-filled syringe with needle shield | 300 mg/2 mL | 0024-5914-01 (pack of 2) |
| Single-dose pre-filled syringe (without needle shield) | 300 mg/2 mL | 0024-5916-01 (pack of 2) |
| Condition | Specification |
|---|---|
| Refrigerated storage | 36–46°F (2–8°C); store in original carton, protected from light |
| Room temperature storage | ≤77°F (25°C) for maximum 14 days; discard if >14 days at room temperature |
| Prohibited conditions | Do NOT freeze. Do NOT expose to heat. Do NOT shake. Do NOT expose to direct sunlight. |
| Pre-injection | Allow to reach room temperature (≥45 minutes before injection; do not use external heat source) |
| Preservative | None — discard any unused portion |
| Population | Guidance |
|---|---|
| Pregnancy | No human data available. Human IgG4 crosses the placental barrier; fetal exposure possible. No adverse developmental effects in cynomolgus monkeys at doses up to 10× MRHD through organogenesis to parturition. Benefits vs risks must be assessed individually. |
| Lactation | No data on dupilumab presence in human milk. Human IgG present in breast milk. Consider benefits of breastfeeding alongside maternal clinical need. |
| Pediatric (<18 yr) | Safety and efficacy not established at initial approval (2017). [Note: subsequent label updates expanded indication to adolescents and children.] |
| Geriatric (≥65 yr) | 67/1472 subjects ≥65 years in pivotal program. No differences in safety or efficacy observed; however, sample size insufficient for definitive conclusions. No dose adjustment required. |
| Renal impairment | No formal studies; no dose adjustment recommended based on population PK. |
| Hepatic impairment | No formal studies; no dose adjustment recommended. |
| Body weight | Higher body weight associated with lower trough concentrations; clinical significance not established; no weight-based dose adjustment recommended. |
Source: BLA 761055 FDA-approved prescribing information (March 2017). This profile reflects the original approval label; subsequent label supplements have expanded the indication to additional populations and indications (asthma, CRSwNP, EoE, prurigo nodularis, CSU).
| Role | Detail |
|---|---|
| Clinical Reviewer | Brenda Carr, MD |
| Division | Division of Dermatology and Dental Products (DDDP) |
| Office | ODE III (Office of Drug Evaluation III) |
| Applicant | Regeneron Pharmaceuticals, Inc. (BLA holder) / sanofi-aventis U.S. LLC (co-marketer) |
| Reference ID | 4075125 (Clinical Review); 4075926 (Label) |
| Manufacturing | Regeneron Pharmaceuticals, Inc., Tarrytown, NY 10591 (U.S. License No. 1760) |
Postmarketing commitments included: (1) ophthalmological assessments incorporated into an ongoing open-label extension (OLE) study to further evaluate the eye disorder signal; (2) ongoing pharmacovigilance for conjunctivitis, keratitis, and herpes virus infections. The eye disorder signal was considered the primary identified risk, offset by the significant unmet need and favourable benefit-risk profile.
Regulatory timeline based on BLA 761055 clinical review and FDA Drugs@FDA records. Subsequent supplemental approvals are listed for contextual completeness and reflect post-2017 label expansions not covered by the original BLA documents uploaded. For the most current prescribing information visit: https://www.fda.gov/drugsatfda (BLA 761055).